MADISON
Retrun to 22q StoriesYou are here
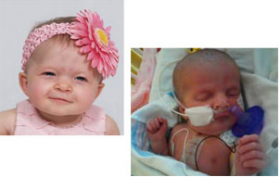
As a mother to two healthy children already, I never expected anything to be different with a new baby. Madison showed us that things don’t necessarily go as expected.
Finding out we were expecting our third child brought a lot of emotions. We had talked about having another child, but never really “decided” to. The pregnancy did not seem much different from the other two, morning sickness and fatigue were really my only troubles.
Around week 16, I just felt so big and was measuring about three weeks ahead. My doctor did not seem to concerned and we all figured it was because I had already had two children. I continued a normal routine of work and home life. When I went in for a routine check up at 24 weeks, my doctor was counting her heart rate and looked a little concerned. He said he thought he heard her heart skipping beats and he wanted me to have an ultrasound done right then.
I waited, nervously, for the sonographer to call me back. She did her scan, in silence, and I waited again. My doctor called me back and said he was concerned about the amount of amniotic fluid around the baby and the risk of me going into pre-term labor.
He referred me to a high risk specialist the next week.
The high risk appointment was very detailed. Medical histories on myself, my husband, our children, and our families, meet the genetic counselor, labs drawn, put on the monitors, ultrasound, 4-D ultrasound, and then finally a discussion with the doctor. That’s when we received the worst news ever — heart defects! The doctor told us that her thought was a genetic disorder called DiGeorge syndrome or 22q11 Deletion. She explained all the possible effects this could have on the baby including heart defects, immune system deficiencies, cleft palate, developmental delays, etc. We were then referred a pediatric cardiologist at the children’s hospital and scheduled a follow up with her after. I didn’t understand how this could be happening to us and our child, I just wanted to fall apart.
I tried to remain optimistic, maybe the scan wasn’t completely correct. I told myself the cardiologist would clear this up and it would not be as bad as it seemed, if only that had been the case! We went to the cardiology appointment, and had another scan done. It took forever! Finally, when it was done, we waited to talk to the cardiologist, hoping for some better news. My heart raced as he started explaining the first defect, then the second, and the third, and fourth, and fifth!
Really!?
How could this be? how could such a little life possibly survive with all this going on? He explained her ASD, VSD, Interrupted Aortic Arch, Bicuspid Aortic Valve, and Aberrant Subclavian Artery. He then went on to explain that she would require open heart surgery after she was born. He told us that there was a duct that normally closes 48 hours after a baby is born, the ductus arteriosus, and that they would have to force the duct to remain open with medications until she could have her surgery. Other issues at hand were that he was not sure if the surgery could be done at our local hospital and she needed to weigh at least 6 pounds for a surgeon to operate. I tried to remain as calm as possible, until we got home and all I could do was cry.
I continued working and taking care of the things I had to do. I went to the follow up high risk appointment and she told us that the labs came back positive for DiGeorge syndrome as discussed at the previous appointment and she scheduled an amniocentesis, to confirm the results and take off some of the excess amniotic fluid. I was placed on modified bed rest shortly after.
I started having contractions around 33 weeks due to the excess fluid and was admitted to the hospital. They were able to stop the contractions with a magnesium sulfate drip and I was sent home a few days later. A couple days after going home, I started having some more mild contractions and called my doctor. I was placed on a home monitor and a turbutaline pump a week or so later.
This did not help — at 35 weeks I was admitted again. This time, the magnesium sulfate did not help, I was contracting through the medication. Madison Grace made her silent arrival June 28, 2010, five weeks early.
She weighed 6 pounds, 1 ounce, an ounce more than she needed for her open heart surgery! She was not breathing, and just as they got ready to intubate her, she started to breathe on her own. She was taken to the NICU right away. I did not get to see or hold her, and wouldn’t hold her until the night before her surgery. Later that evening the cardiac surgeon requested to talk with us in the NICU. He confirmed all the previously discussed defects and let us know that he would not be able to do her surgery, she would have to go to Atlanta — two hours away.
The next morning the neonatologist came in, she needed me to sign a consent to have Madison airlifted to Children’s Hospital of Atlanta. Up until then, I had been doing okay, but at that moment it all became very real to me and I broke down again. I signed her transfer and consent for transporting her. I then called my doctor and requested to be released as soon as possible so I could go home and pack. We also had a visit from the geneticist that morning. He told us that he checked Madison over and he saw some features of Digeorge syndrome, including a cleft palate. I was released later that day. The next morning was very hard, knowing I had to go say bye to my baby girl, even though I would see her later in the day.
We met with the flight nurse and the pilot, who informed us that they did not like the weather so they were transporting her by ambulance. We said our goodbyes and started our way to Atlanta, our new home until further notice!
When we arrived we were able to see her in the CICU, but then had to go register her. When we finished, we went back to her bedside. We watched nurses, x-ray technicians, sonographers come and go, running test after test. Finally that night we talked to one of the Fellows working on her case. He confirmed all of her defects again and explained that the surgeon thought it would be necessary for Madison to have the Norwood procedure done.
This procedure was explained to us in detail by the cardiologist we originally saw back home, so this is what we were expecting. We were also told that Madison was one of the less “severe” cases they had at that time and it would be a couple days before she would be in the operating room. That Saturday, July 3, we met with the surgeon, the chief of cardio-thoracic surgery, we felt really good about the plan and were happy that we had the head of the team working with our daughter. With Sunday being a holiday, and Monday being the day the hospital took, her surgery would not be until Tuesday. However, Monday morning we had a visit from the assistant chief surgeon. He told us that the other surgeon had another baby come in that he had been following in utero, and that he would be taking over Madison’s care. He then proceeded to tell us that he felt a complete repair of the arch, ASD, and VSD was possible. This was great news, but not what we were prepared for. We had already accepted that she would need other surgeries and we accepted the risks involved. He explained that if he got in and saw that the repair was not possible, then he would do the Norwood as previously planned. That night we finally got to hold her for the first time — it was a very sleepless night!
The next morning we arrived early as planned and spent a little time with Madison before her surgery. We signed all her consents and talked to her surgical team. We walked her to the OR, kissed her, and handed her off to the anesthesia team. Then we waited, the longest and most stressful wait I will probably ever have! Every hour an nurse called and gave us an update. One hour passed, two hours, three, five, seven, finally after eight hours our surgeon came in. It went well, they were able to do a complete repair for her and she was doing great. They were unable to close her chest due to swelling, but he said it was normal. We would be able to see her soon. It was about 30 minutes longer and they let us see her for a minute, there was a patient having a problem and did not allow any visitors in the CICU when that happened.
She looked okay,she had several chest tubes in draining fluid, she was still intubated and they were keeping her “out” until they closed her chest, and was definitely swollen, but better than I expected. When we went back to see her that night, I broke down again. She looked so pitiful and I was hurting for her. Everytime I looked at her my heart broke and I cried!
The next morning was easier, she looked better. The swelling started to come down and they promised that she wasn’t in any pain. They were able to close her chest two days after her surgery, and her recovery went well. She was moved to the step down unit about a week later, and we got to take her home a week after that.
In the months following her discharge, Madison also had surgery on her airway, stomach, cleft palate, G-Tube placed, heart catheterization, and aortic valvuloplasty. Aside from Madison’s heart defects her other 22q characteristics include compromised immune system, feeding/swallowing difficulties, failure to thrive, laryngomalacia (treated), hypocalcemia (resolved), severe reflux, nasal regurgitation (resolved), droopy eyelids, weak tooth enamel and developmental delays. She currently goes to speech/feeding therapy, occupational therapy, and physical therapy. She is only taking baby aspirin daily and is doing better than expected at this time. She is such a strong little girl and has taught myself and our family so much already. We are looking forward to everything she has yet to show us!